Limited Time Offer
50% off Ketamine Companion Membership for 6 Months. Learn more about membership
What Does Ketamine Do to You: Brain and Body
Summary
Ketamine works differently than traditional treatments, affecting both the brain and body in ways that can rapidly shift mood, perception, and pain. It may support neuroplasticity and help break stuck patterns, but results vary and there are important risks to consider. Understanding how ketamine works, both short and long term, can help you approach treatment more intentionally and safely.
Ketamine is a name you might have heard in different contexts. Originally, it was used as an anesthetic in medical settings. However, its role has expanded beyond the operating room. People often wonder what does ketamine do to you, especially as clinical uses grow.
In recent years, ketamine has gained attention for its potential mental health benefits. It is being studied for its rapid-acting antidepressant effects. This has sparked interest among researchers and healthcare professionals alike.
Understanding what ketamine does to your brain and body is crucial. It helps in making informed decisions about its use. Ketamine works in complex ways, affecting various brain systems. Put simply, what does ketamine do to the brain and how does ketamine affect the brain across short- and long-term use are core questions researchers study.
The brain is a complex organ, and ketamine interacts with it in unique ways. It blocks certain receptors, leading to changes in brain chemistry. These changes can influence mood, perception, and even pain. These shifts are central to how ketamine works in the brain.
Ketamine’s effects are not limited to the brain. It also impacts the body, sometimes causing dissociation, altered perceptions, or temporary altered states of consciousness that can affect mood, awareness, and sensory processing. Collectively, these ketamine effects on brain and body can vary widely among individuals.
The potential benefits of ketamine are promising, but there are risks too. Long-term use can lead to cognitive impairments and other health issues. Therefore, understanding both sides is essential.
As research continues, ketamine's role in mental health treatment is evolving. It offers hope for those with treatment-resistant conditions. However, it is important to approach its use with caution and professional guidance. Ongoing trials aim to clarify 'what does ketamine do to the human brain' in clinical settings and real-world care. If you want to learn more about the real world care, check out our resource on ketamine therapy.
What is Ketamine? A Brief Overview
Ketamine is a dissociative anesthetic developed in the 1960s. Initially, it was used extensively in veterinary medicine and human anesthesia. Its unique properties made it valuable in emergency and battlefield settings.
Over time, ketamine's use extended beyond anesthesia. Researchers discovered its potential for treating mood disorders. Its fast-acting nature offers potential relief for depression and PTSD.
Understanding ketamine involves grasping its chemical and functional diversity. Here's a brief look:
- Anesthetic: Originally for surgery, reducing pain and consciousness.
- Dissociative: Alters perception of reality, sometimes used recreationally.
- Therapeutic: Investigated for mental health benefits, such as depression alleviation.
Ketamine works by interacting with NMDA receptors in the brain. This interaction leads to increased glutamate levels. Glutamate is crucial for brain processes like learning and memory, which helps explain how ketamine works in the brain.
Despite these benefits, the recreational use of ketamine carries risks. It can cause hallucinations and other sensory distortions. Therefore, its usage needs careful oversight, especially in therapeutic contexts.
Ketamine's medical and therapeutic roles continue to expand with research. However, distinguishing between its medical use and potential for misuse is important. Understanding its full range of effects can aid in evaluating its role in health care.
How Ketamine Works in the Brain: The Science Explained
So, how does ketamine work in the brain? Ketamine's impact on the brain is both fascinating and complex. It acts primarily by blocking NMDA receptors, a type of receptor for the neurotransmitter glutamate. By doing so, ketamine increases the amount of glutamate in the brain. These ketamine brain mechanisms are key to its therapeutic effects.
This surge in glutamate is key. Glutamate is a major neurotransmitter involved in synaptic plasticity, which is how our brains adapt and learn. Ketamine indirectly boosts the brain's ability to forge new connections between neurons. These ketamine brain pathways are tied to learning and mood.
Furthermore, ketamine's effect on glutamate is thought to enhance mood regulation. This is critical for treating conditions like depression and anxiety. For many, ketamine can relieve depressive symptoms within hours.
Research into ketamine shows changes in brain activity patterns. It can help break unhealthy thought loops common in depression. This disrupts patterns and allows for healthier mental habits to form.
Interestingly, ketamine works differently from traditional antidepressants. While most take weeks to have an effect, ketamine acts quickly. This rapid response makes it a promising option for those with treatment-resistant depression.
However, the exact mechanisms behind ketamine's mental health benefits are still being explored. Scientists are exploring how ketamine might repair or reinforce neural pathways damaged by chronic stress. This research holds hope for more effective mental health treatments.
Ketamine may also influence other neurotransmitter systems. Studies are exploring its effects on dopamine and serotonin, which are closely linked to mood and emotion. Understanding these effects will further clarify ketamine's role in mental health care.
A closer look at ketamine's brain mechanisms reveals several key points:
- NMDA Receptor Blockade: Increases glutamate, promoting plasticity.
- Brain Connectivity: Enhances neural connections for mood stability.
- Rapid Response: Fast-acting, especially compared to traditional treatments.
- Neurotransmitter Influence: May affect serotonin and dopamine.
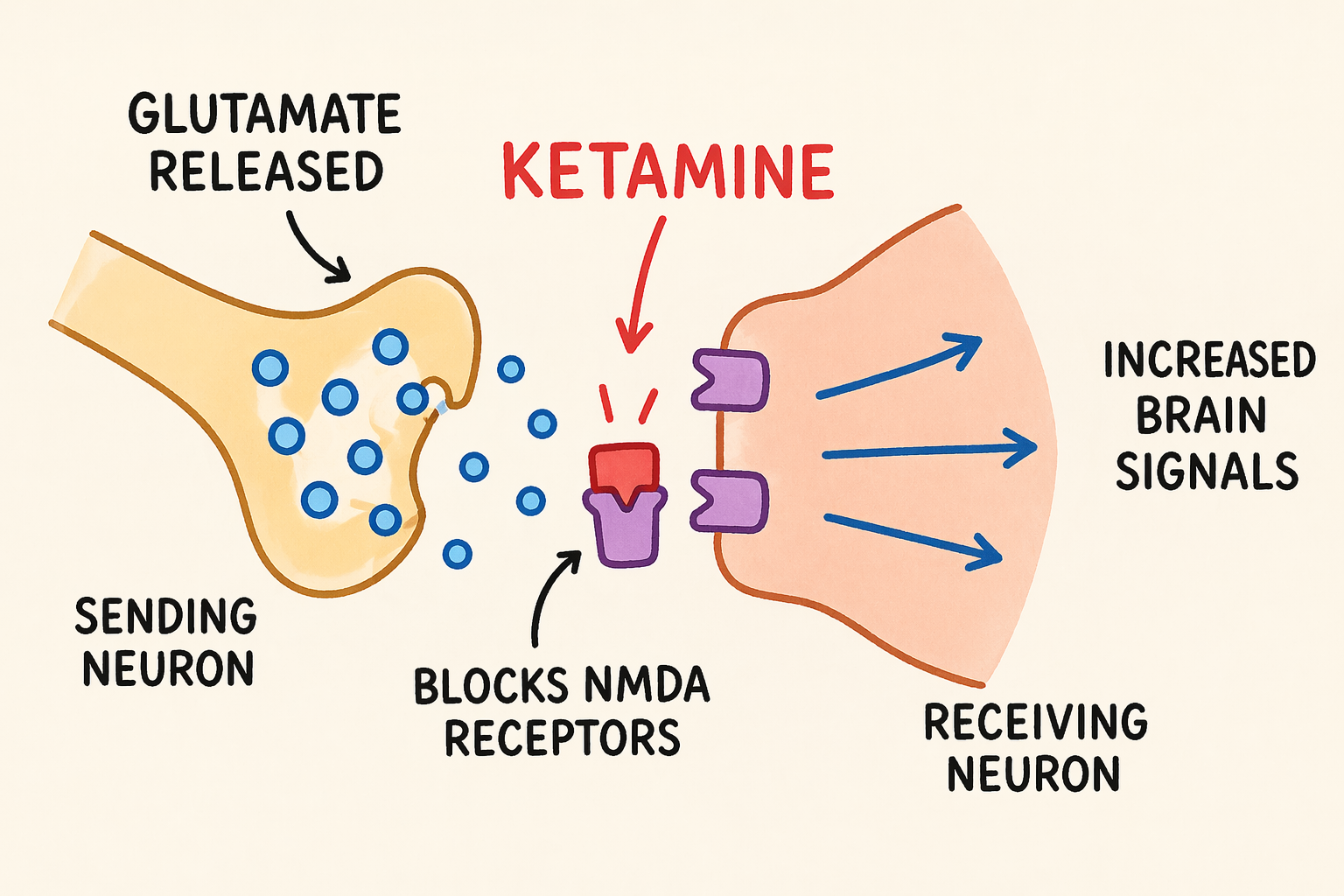
Understanding ketamine requires blending knowledge of neurobiology and mental health. As research advances, so does the possibility of integrating ketamine into broader therapeutic strategies. This could reshape how we approach and treat mental health disorders.
Ketamine's Effects on Brain Chemistry and Neuroplasticity
Ketamine plays a remarkable role in altering brain chemistry. It primarily targets glutamate pathways, one of the most abundant neurotransmitters in the brain. By enhancing glutamate action, ketamine can influence how information is processed and communicated in the brain.
Glutamate's role is pivotal for neuroplasticity. Neuroplasticity refers to the brain's ability to reorganize itself by forming new neural connections. This is crucial for learning, memory, and recovery from brain injuries.
Ketamine acts as a catalyst for synaptic plasticity. It triggers a cascade of chemical events that allow neurons to form more connections. This boost in connectivity can help restore normal function in depressed or traumatized brains. Some describe these restorative changes as ketamine brain repair, though the term is informal and still under investigation.
Interestingly, ketamine affects the expression of Brain-Derived Neurotrophic Factor (BDNF). BDNF is a protein that supports neuron growth and survival. Higher levels of BDNF are associated with improved brain health and function.
Alterations in BDNF levels can impact mood and resilience to stress. By potentially elevating BDNF, ketamine may enhance the brain's ability to cope with stressors. This could explain why ketamine is being explored for various psychiatric conditions.
Moreover, ketamine's effects go beyond just neurotransmitters. It can also influence brain networks and regions, particularly those linked to mood and cognition. This makes ketamine a unique tool in addressing mood disorders.
These insights into ketamine's effects on brain chemistry illuminate several key areas:
- Boosts Glutamate: Enhances the brain's main excitatory neurotransmitter.
- Enhances Neuroplasticity: Promotes synaptic connections for healthier brain function.
- Increases BDNF: Supports growth and repair of neurons.
- Impacts Mood Networks: Alters brain regions tied to emotion and thought.
Understanding the impact of ketamine on neuroplasticity and brain chemistry opens new avenues for therapeutic interventions. As research progresses, the potential to heal through ketamine grows. It might reshape how we tackle mental health and neurodegenerative disorders.
How Does Ketamine Rewire Your Brain?
The concept of 'rewiring' your brain may sound like science fiction, but with ketamine, it's grounded in scientific exploration. Ketamine's influence on brain plasticity is central to this phenomenon.
Ketamine stimulates the growth of new synapses, the junctions where neurons communicate. This synaptogenesis aids in developing fresh pathways, akin to constructing new roads for better connectivity. These new connections can lead to improved cognitive and emotional processing.
One of the key players in this process is ketamine's ability to modulate NMDA receptors. These receptors are crucial for synaptic plasticity and learning. When ketamine blocks NMDA receptors, it encourages the brain to form new networks, creating pathways for healing and adaptation.
Interestingly, ketamine also influences the default mode network (DMN). The DMN is involved in self-referential thinking and is active when the mind is at rest. Alterations in DMN connectivity are associated with mood disorders. Ketamine can help recalibrate this network, leading to increased emotional resilience.
This rewiring might lead to transformative outcomes in mental health treatment. By fostering brain circuits' repair and regeneration, ketamine may provide renewed hope for those battling chronic depression or post-traumatic stress. This helps explain why some ask, is ketamine good for your brain, particularly when considering resilience and recovery.
In summary, ketamine's role in brain rewiring involves several vital elements:
- Synaptogenesis: Formation of new synapses, enhancing brain connectivity.
- NMDA Receptor Modulation: Encourages new neural pathways by blocking specific receptors.
- Default Mode Network Adjustment: Resets networks influencing mood and self-reflection.
Through these mechanisms, ketamine may do more than treat symptoms---it might fundamentally change how the brain operates. This potential rewiring underscores ketamine's promise as a therapeutic agent in mental health care. As research expands, its full potential may soon be realized.
The Physical Effects of Ketamine on the Body
While ketamine is known for its profound effects on the brain, its impact on the body is equally significant. When administered, it engages with the body's systems in various ways.
Ketamine acts primarily as an anesthetic, which means it works by numbing perception of pain. This numbing effect can extend to a complete dissociation from the physical body at higher doses. Users may feel disconnected from their physical presence, which is why it's termed a 'dissociative' anesthetic.
The immediate physical reactions to ketamine can include increased heart rate and blood pressure. These effects are usually temporary, occurring during the onset of the drug. As the effects peak, users might experience muscle relaxation or, conversely, body stiffness.
Ketamine can also affect the respiratory system. While it generally maintains respiratory function, some individuals might experience slowed breathing. Therefore, monitoring is crucial during administration, especially in controlled settings.
Ketamine side effects can vary greatly depending on dose and personal health. High doses might lead to unwanted physical reactions such as nausea or vomiting. Understanding these potential outcomes helps in managing expectations and safety.
In summary, the physical effects of ketamine encompass:
- Pain Perception: Reduces sensation through dissociative anesthetic properties.
- Cardiovascular System: Increases heart rate and blood pressure.
- Respiratory Effects: Rarely slows breathing; generally maintains function.
It's crucial to be aware of these physical effects when considering ketamine therapy. Each reaction offers insights into how ketamine interacts with the body's intricate system, underscoring the necessity for professional oversight in therapeutic contexts. Understanding these impacts can help mitigate risks and ensure a safer experience for those exploring ketamine's therapeutic benefits.
Short-Term Effects: What Happens When Someone is on Ketamine?
When someone on ketamine begins to feel the effects, changes can appear quickly. These effects vary based on the dose and individual sensitivity.
A common sensation is dissociation, where the person feels detached from their surroundings. This may lead to a dreamlike state or sense of floating. For some, this detachment provides a relief from persistent stress or emotional burden.
In addition to dissociation, sensory perceptions can change. Some people report visual or auditory distortions, including intensified colors or sounds. These altered consciousness perceptions can contribute to the hallucinogenic experience often associated with ketamine.
Physical sensations may also shift while under ketamine's influence. Relaxed muscles, or conversely, muscle rigidity, can occur. Some individuals experience a sense of heaviness or lightness in their limbs.
Emotional responses during a ketamine experience can range widely. While many find it mood-enhancing, others might feel anxious or confused. Monitoring and a safe setting can reduce the risk of distress during this time.
To summarize, short-term effects of ketamine include:
- Dissociation: Feeling detached from the environment.
- Sensory Alterations: Visual/auditory distortions.
- Physical Sensations: Muscle relaxation or rigidity.
- Emotional Variability: From euphoria to anxiety.
Understanding these short-term effects helps prepare both patients and practitioners for safe and effective administration. Recognizing the spectrum of experiences guides the therapeutic use of ketamine, ensuring its benefits are maximized and risks minimized.
Long-Term Effects: Risks and Potential Benefits
The impact of ketamine extends beyond its immediate effects. Long-term use carries both potential benefits and risks that should not be overlooked.
Research indicates ketamine might support brain health by promoting neuroplasticity. This could involve forming new neural connections, potentially aiding in healing from depression or trauma.
Yet, frequent use of ketamine can pose serious risks. Cognitive impairments like memory issues have been noted among regular users. Such changes can affect daily functioning and overall mental clarity over time.
Bladder health is another concern with prolonged ketamine use. Chronic exposure has been linked to urinary tract issues, sometimes severe enough to require medical intervention.
On the positive side, ketamine's ability to swiftly reduce depressive symptoms is a significant therapeutic advantage. This offers hope for individuals unresponsive to conventional antidepressants, reshaping mental health treatment paradigms.
However, the risk of addiction cannot be dismissed. Recreational misuse of ketamine raises concerns about dependency, emphasizing the need for controlled, clinical oversight. Researchers also continue to study what does ketamine do to the human brain with repeated exposure.
The potential benefits and risks of ketamine's long-term use can be summarized as follows:
- Neuroplasticity: Enhances neural connectivity.
- Cognitive Risks: Potential for memory impairments.
- Bladder Health: Possible urinary complications.
- Rapid Antidepressant Action: Benefits treatment-resistant depression.
- Addiction Risk: Raises concern for misuse.
Balancing these factors is crucial for those considering ketamine therapy. Ongoing research continues to refine our understanding of its long-term effects, aiming to harness its therapeutic promise while mitigating risks. Both patients and healthcare providers must remain informed and vigilant about these considerations.
Ketamine for Mental Health: Depression, PTSD, and Beyond
In recent years, ketamine has been spotlighted for its potential in mental health treatment. It offers unique advantages where traditional methods fall short.
One of the most profound impacts of ketamine is ketamine for depression treatment. Many patients experience relief within hours, a stark contrast to the weeks required for conventional antidepressants to take effect.
For those with PTSD, ketamine shows promise as well. It appears to soothe symptoms by affecting brain regions involved in emotion regulation and fear responses.
Research also explores ketamine's role beyond depression and PTSD. Anxiety disorders and chronic pain management are areas where ketamine could be beneficial.
The scope of ketamine's applications in mental health is vast:
- Depression: Rapid symptom relief for treatment-resistant cases.
- PTSD: Potential reduction in anxiety and fear-based symptoms.
- Anxiety Disorders: Early studies suggest possible relief.
- Chronic Pain: Investigated for its potential analgesic properties.
Despite these promising findings, ketamine therapy isn't suited for everyone. Patient history and potential side effects must be carefully considered before determining if someone is a good fit.
The broader acceptance of ketamine in mental health care hinges on continued research. Studies aim to unravel its mechanisms and optimize dosage and administration methods. As understanding grows, so does hope for millions struggling with persistent mental health challenges. The evolving landscape of ketamine therapy holds potential to redefine treatment protocols, offering new avenues for healing.
Want to dig deeper? Read our article What is Ketamine Therapy.
Is Ketamine Good for Your Brain? Weighing the Pros and Cons
The question of whether ketamine is beneficial for the brain is complex. On one hand, it's hailed for its rapid antidepressant effects. Many individuals with treatment-resistant conditions have found renewed hope through ketamine.
However, there are concerns about long-term use. Frequent use can lead to cognitive impairments and other health issues. Therefore, it's crucial to weigh both the positive and potential negative outcomes.
It's essential to understand ketamine's dual nature:
- Pros :
- Rapid relief from depressive symptoms.
- Potential to promote brain repair and neuroplasticity.
- Effective in treatment-resistant cases.
- Cons :
- Risk of cognitive decline with prolonged use.
- Potential for addiction and misuse.
- Side effects such as hallucinations.
The decision to use ketamine should be made carefully, guided by professional advice. Each individual's situation is unique and deserves a tailored approach. By considering both sides, patients and practitioners can make informed decisions about incorporating ketamine into treatment plans. This process should always prioritize safety and long-term well-being over short-lived benefits.
Safety, Side Effects, and Who Should Avoid Ketamine
Safety is a crucial concern when considering ketamine therapy. While many people experience positive results, the risk of side effects exists. Common side effects include nausea, dizziness, and increased heart rate. Hallucinations and dissociative experiences may also occur.
Certain individuals should avoid ketamine. Those with a history of substance abuse, for instance, may be at higher risk for addiction. Ketamine can also interact poorly with certain medications and medical conditions.
Before starting ketamine therapy, thorough evaluation is key. Healthcare professionals assess each patient's health history and current medications. This ensures that ketamine is a suitable choice.
- Avoid ketamine if :
- You have a history of severe substance abuse.
- You have uncontrolled hypertension or heart disease.
- You are pregnant or breastfeeding.
Professionals must carefully monitor those receiving ketamine treatments. Regular follow-up appointments help ensure safety and effectiveness. By staying vigilant about potential side effects, individuals can make the most of ketamine therapy while minimizing risks.
The Future of Ketamine Therapy: Research and Hope
The future of ketamine therapy shines with promise. Ongoing research aims to refine its use in treating mental health disorders. Studies are exploring how to maximize benefits while minimizing side effects. This research could transform how we approach mental health care.
New formulations and delivery methods are under investigation. Researchers are working on ketamine analogs that offer therapeutic benefits with fewer risks. Innovations in delivery, such as controlled ketamine infusion, are enhancing precision in treatment.
Emerging evidence suggests ketamine may treat conditions beyond depression. Anxiety disorders, PTSD, and bipolar disorder are potential targets. These possibilities expand the scope of ketamine's impact on mental health.
- Key areas of focus :
- Developing safer ketamine analogs.
- Exploring new applications for various mental health conditions.
- Improving precision in dosing and delivery methods.
The hope is that ketamine therapy will become a mainstream option, accessible to more people. With continued research and understanding, ketamine could represent a paradigm shift in mental health treatment. The journey towards this future is filled with potential and optimism.
Explore Programs
Limitless Ketamine Therapy Mindset Companion Membership

Maximize treatments with Limitless ketamine mindset companion and monthly courses to support your ketamine therapy journey.
Key Takeaways: What You Need to Know About Ketamine and Your Brain
Ketamine's effects on the brain are profound, offering hope for mental health treatments. Its ability to work rapidly sets it apart from traditional therapies. Many are drawn to its potential for treating severe depression swiftly.
Understanding how ketamine rewires the brain helps address misconceptions. This drug enhances neuroplasticity and encourages new neural connections. Research is uncovering how this process improves mood and well-being.
However, ketamine therapy is not without risks. It's crucial to consider potential side effects, such as hallucinations or cognitive changes. Long-term use can also pose issues like dependency or bladder harm.
- Critical Points :
- Ketamine acts fast, particularly in treatment-resistant depression.
- It promotes neuroplasticity, potentially rewiring the brain.
- Possible risks: cognitive impacts and physical side effects.
- Clinical guidance is essential to ensure safe use.
Ketamine's future in mental health care is promising, with ongoing research expanding its applications. Informed decision-making involves weighing benefits against risks. Understanding these factors equips you to engage meaningfully in discussions about ketamine and brain health.
Ketamine can change how you experience your body, thoughts, emotions, and surroundings. Some people feel relaxed, detached, dreamlike, or more distant from difficult thoughts. These effects vary by dose, setting, and individual response.
Ketamine affects the brain’s glutamate system and NMDA receptors, which may support neuroplasticity and changes in mood, perception, and pain processing. In the body, it may temporarily increase heart rate or blood pressure and can cause nausea, dizziness, or dissociation.
Ketamine works in the brain by blocking NMDA receptors and influencing glutamate activity. This may help the brain form new neural connections, which is one reason researchers study ketamine effects on brain function, mood, and treatment-resistant depression.
When people ask how does ketamine rewire your brain, they’re usually referring to neuroplasticity. Ketamine may help create a window where the brain becomes more flexible, allowing new patterns of thought, emotion, and response to form with proper support.
Ketamine may offer benefits for some people when used medically, especially for treatment-resistant depression. But it is not risk-free. Frequent or unsupervised use can carry risks, including cognitive changes, bladder issues, dependency, and other side effects. Clinical guidance matters.
Ketamine primarily blocks NMDA receptors, which increases glutamate, the brain’s main excitatory neurotransmitter, leading to enhanced synaptic plasticity and stronger neural connections. This surge in plasticity can rapidly disrupt unhealthy thought loops and stabilize mood, often relieving depressive symptoms within hours, unlike traditional antidepressants that take weeks. Researchers are also exploring ketamine’s influence on other systems like serotonin and dopamine to better understand its fast-acting effects.
“Rewiring” refers to ketamine’s ability to promote synaptogenesis, the growth of new synapses, by modulating NMDA receptors and boosting neuroplasticity. It can also help recalibrate the default mode network (DMN), which is tied to self-referential thinking and mood. Together, these changes can create healthier neural pathways that support improved emotional processing and resilience.
Short-term effects often include dissociation (feeling detached or dreamlike), changes in sensory perception (visual or auditory distortions), and shifts in physical sensations (muscle relaxation or rigidity). Heart rate and blood pressure may temporarily rise, and while breathing is generally maintained, careful monitoring is important. Emotional responses can range from calm or uplifted to anxious or confused, so a safe, supervised setting matters.
Potential benefits include rapid relief of depressive symptoms and enhanced neuroplasticity that may help repair mood-related circuits. Risks with frequent or prolonged use include cognitive impairments (such as memory issues), bladder and urinary problems, and the possibility of addiction or misuse. Because of this risk–benefit balance, ketamine should be used with clinical oversight and individualized treatment planning.
People with a history of severe substance abuse, uncontrolled hypertension or heart disease, or those who are pregnant or breastfeeding should avoid ketamine. It can also interact with certain medications and medical conditions, so a thorough evaluation of health history and current treatments is essential. Professional guidance and ongoing monitoring help ensure safety and effectiveness.